Our teeth are strong, but they can break for many reasons, for example, tooth decay, injury, or teeth grinding. And when they do, it’s not always easy to fix them. If you have diabetes, you’re at an increased risk for tooth breakage and other oral health problems. In this blog post, We will discuss the link between diabetes and teeth breaking and what you can do to prevent it from happening.
What Causes Tooth Breakage?
There are many reasons why teeth can break, but the most common cause is tooth decay. When bacteria build up on your teeth, it creates an acidic environment that can break down the tooth enamel. This process is called demineralization, which weakens the tooth and makes it more susceptible to breakage. Other causes of tooth breakage:
- Biting hard objects such as ice
- Chewing on hard foods such as candy
- Using your teeth as tools, for example, to open a bottle
- Grinding your teeth (bruxism)
- Injury to the mouth or teeth, for example, from a fall or sports injury.
All of these activities can put stress on the teeth and cause them to break. However, diabetes can lead to the breaking of your teeth even without any of these activities, but why?
The Link Between Diabetes and Teeth Breaking
As we mentioned, tooth decay is the most common cause of tooth breakage. Diabetes increases your risk for tooth decay through several mechanisms.
- Diabetes decreases the salivary flow, which helps to neutralize the acids in your mouth and keep bacteria levels under control.
- Medications used to treat diabetes can cause dry mouth. Saliva neutralizes acids produced by bacteria and promotes remineralization, a natural tooth repair process.
- High levels of glucose in blood and saliva also provide an ideal environment for bacterial growth.
- Diabetes increases the risk of gum pockets, which cause the accumulation of food debris and bacteria around the teeth. You can read more about pockets between teeth and gums.
All of these factors put people with diabetes at an increased risk for tooth decay and make their teeth prone to fracture.

Why Your Teeth Are Breaking If You Have Diabetes?
Saliva is important for keeping your mouth healthy. It helps remove food and bacteria from your teeth and contains minerals that can help remineralize the tooth enamel. When you have diabetes, your saliva production may decrease, leading to dry mouth (xerostomia). This can make it more difficult to remove food and bacteria from your teeth, causing tooth decay. Tooth decay is the most common cause of tooth breakage. A dry mouth condition may also occur as a side effect of some diabetes medications.
In addition, tooth decay bacteria feed on sugar, and people with diabetes often have high blood and saliva glucose levels. This can create an environment for bacteria to thrive, causing tooth decay.
People with diabetes are also at an increased risk for gum disease. Gum disease is an infection of the gums that can cause them to pull away from the teeth, creating gum pockets in which bacteria can grow. These pockets, also known as periodontal pockets, cause the accumulation of bacteria and food debris between teeth, causing tooth decay and breakage. Gum disease can also lead to the loss of bone and tissue around the teeth, which can eventually lead to tooth loss.
You can read more about how does diabetes affect your teeth and oral health?
Treatment of Broken Teeth
If you have diabetes and your teeth are breaking, you must see your dentist as soon as possible. Depending on the severity of the break, your dentist may recommend one of the following treatments:
- Dental bonding: This is a quick and easy procedure in which your dentist applies a tooth-colored resin to the broken tooth. The resin is then hardened with ultraviolet light and bonds to the tooth to restore its shape and strength.
- Root canal treatment: This is a procedure in which the dentist removes the damaged tooth pulp, cleans and disinfects the tooth, and then fills it with a rubber-like material. Root canal treatment is used to save teeth with severe decay or infection.
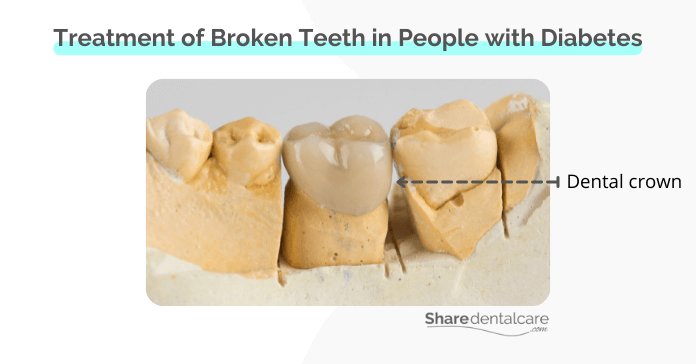
- Dental crowns: A crown is a custom-made, tooth-shaped cap that covers the entire surface of a tooth. They are used to restore the shape, size, and strength of a tooth that has been damaged by decay or injury. You can read more about teeth caps for adults.
- Tooth extraction: In some cases, a tooth may be so badly damaged that it needs to be removed. Your dentist will only recommend this as a last resort. After that, your dentist may recommend that you replace the missing tooth with a dental bridge or implant.
Prevention of Teeth Breaking in People with Diabetes
There are several things you can do to prevent your teeth from breaking if you have diabetes:
- Control your diabetes by keeping your blood sugar levels under control.
- Brush your teeth twice a day with fluoride toothpaste.
- Floss your teeth every day.
- Eat a healthy diet and avoid sugary snacks.
- Drink plenty of water to keep your mouth hydrated.
- Quit smoking because smoking can damage your teeth.
- See your dentist regularly for checkups and cleanings.
If you have diabetes, it’s essential to take good care of your teeth to prevent them from breaking.
Diabetes and Teeth Breaking – Conclusion
Tooth decay is the most common cause of tooth breakage in people with diabetes. Diabetes can cause dry mouth, which increases the risk of tooth decay. In addition, people with diabetes often have high glucose levels in their blood and saliva, which can create an environment in which tooth decay bacteria can thrive. To prevent your teeth from breaking, it’s important to control your diabetes, brush and floss your teeth regularly, and see your dentist for checkups and cleanings.