Smoking tobacco has harmful effects on your oral health and general health. Gum disease is an infection of the gums that can result in inflammation of the gums, pain, and tooth loss. Smoking tobacco is one of the most common causes of gum disease. According to the centers for disease control and prevention (CDC), smokers have twice the risk for gum disease than non-smokers. In this blog post, we will discuss how smoking tobacco can cause gum disease and how to treat it.
What is Gum Disease?
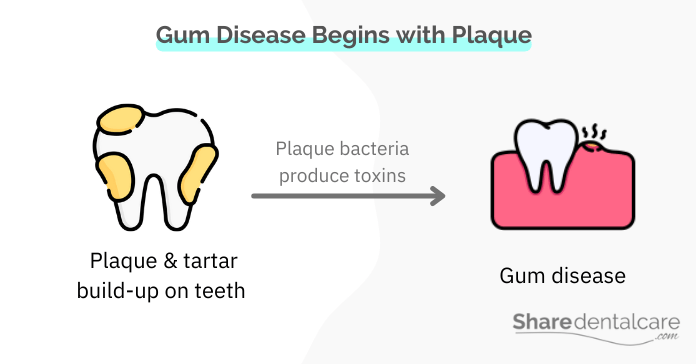
Gum disease, also known as periodontal disease, is an infection of the gums that occurs due to poor oral hygiene and plaque build-up on the teeth. The bacteria in plaque and tartar produce toxins and cause inflammation of the gums. Gum disease is a common problem, affecting more than 47.2% of adults aged 30 years and older. Smoking tobacco allows plaque bacteria to grow, multiply, and get out of control, causing gum disease, which can be categorized into:
- Gingivitis: gingivitis infection is the most common and mild form of gum disease, characterized by red and swollen gums that bleed easily.
- Periodontitis: it is the more advanced form of gum disease, which can lead to tooth loss if not treated.
Signs & Symptoms
The signs and symptoms of gum disease may vary depending on the type of gum disease. The most common symptoms of gum disease are:
- Red, swollen gums.
- Bleeding gums, especially when brushing or flossing your teeth.
- Bad breath that doesn’t go away.
- Receding gums and infected gum pockets.
- Pain with chewing.
- Pus between teeth and gums (gum abscess).
- Change in the way teeth fit together when you bite.
- Loose teeth & tooth loss.
How Does Tobacco Smoking Cause Gum Disease?
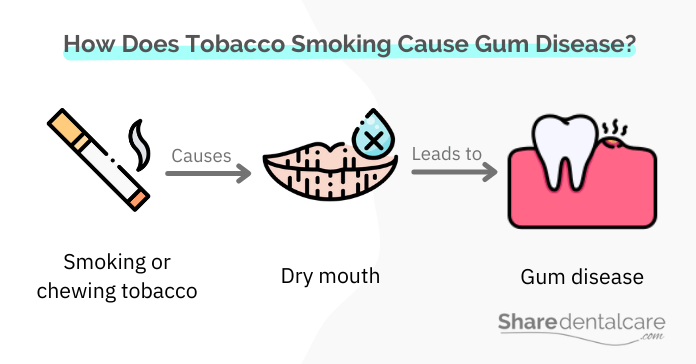
Smoking tobacco is one of the most common causes of gum disease. The chemicals in tobacco smoke cause inflammation of the gums and increase the risk of gum disease. Also, smoking tobacco contributes to dry mouth, which makes it harder for your mouth to fight infection. Saliva helps to wash away plaque and bacteria from the teeth, so when you have a dry mouth, there is an increased risk of developing gum disease.
Smoking tobacco also reduces the blood flow to the gums, which hinders the healing process. Besides, smoking weakens the immune system, making it harder for your body to fight infection and inflammation. According to the centers for disease control and prevention (CDC), smokers have twice the risk of gum disease than non-smokers. Read more about smoking damage to teeth.
Other Causes & Risk Factors
In most cases, gum disease begins with dental plaque. However, several factors can increase the risk of gum disease, including:
- Poor oral hygiene.
- Hormonal changes during puberty, pregnancy (pregnancy gingivitis), and menopause.
- The risk increases with age. 70% of adults 65 years and older have gum disease.
- Certain medications reduce the flow of saliva in your mouth, causing gum disease.
- Systemic diseases such as diabetes mellitus, rheumatoid arthritis, and Crohn’s disease.
- Conditions such as leukemia, and HIV/AIDS, which cause decreased immunity
Health Problems Linked to Smoking Tobacco & Gum Disease
Both tobacco smoking and gum disease can harm your health. They are linked to some serious health problems such as heart attack, stroke, and other serious cardiovascular events. Smokers have a 4 times greater risk of developing heart disease and stroke than nonsmokers.
Gum disease is a risk factor for the development of cardiovascular diseases because it increases inflammation in your body and increases your blood pressure. This can lead to a heart attack or a stroke. The good news is that you can reduce the risk by quitting smoking tobacco and treating gum disease.
Treating Gum Disease & Quitting Tobacco Smoking
The good news is that gum disease can be easily treated and prevented if you quit smoking tobacco. It’s never too late to start living a healthier and smoke-free life. The treatment of gum disease depends on the severity of the condition. In most cases, good oral hygiene and professional teeth cleaning can help to treat the condition.
If you have severe gum disease, you may need to see a dentist or periodontist for treatment, which may include:
- Scaling and root planing: This is a deep cleaning procedure that removes plaque and tartar (hardened plaque) from below the gum line and smoothes the rough edges of the tooth root to decrease inflammation.
- Surgical Treatment: This may involve flap surgery or removal of gum tissue around your teeth. The type of surgery you need will depend on the stage, depth, and severity of your gum disease. Read more about reversing periodontal disease bone loss.
Tobacco smoking will continue to increase your risk of developing gum disease and other health problems. The best way to reduce these risks is to quit smoking tobacco. If you can’t, at least smoke in moderation and try to cut down on the number of cigarettes you smoke each day. Read more about how gums heal after quitting smoking.
Gum Disease from Tobacco – Conclusion
If you’re a smoker, there’s no doubt that smoking is bad for your overall health. Smoking tobacco can also affect your oral health by causing gum disease. Smokers have twice the risk of developing gum disease than non-smokers. Gum disease is an infection of the gums that can cause tooth loss if left untreated. It is also linked to other serious health problems such as heart attack and stroke. The good news is that gum disease can be treated and prevented if you quit smoking tobacco. It’s never too late to start living a healthier and smoke-free life.